Reviewed By: Dr. Miliken
Vision changes rarely announce themselves in a single dramatic moment. More often, it starts as a slight friction that builds. Headlights feel harsher at night. Print looks slightly softer. One eye seems to “do more work” than the other. Two of the most common causes of those shifts are cataracts and glaucoma, and they matter for the same reason: both are common, both can worsen over time, and timely treatment can protect vision.
Cataracts cloud the eye’s natural lens, reducing image clarity. Glaucoma damages the optic nerve and gradually impairs visual function, often starting at the edges. Cataract-related blur is usually reversible with surgery. Glaucoma-related vision loss is not. That distinction is a core consideration when deciding when to get checked and determining if it’s cataracts vs glaucoma.
Table of Contents
What is the difference between cataracts and glaucoma?
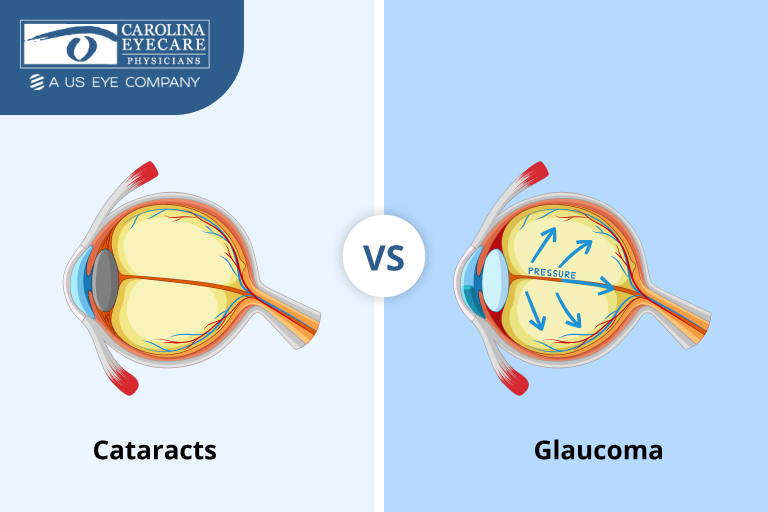
A cataract is a lens problem. The lens is supposed to be clear so light can focus sharply on the retina. Over time, lens proteins can clump and form a haze that scatters light.
Glaucoma is an optic nerve problem. It is often associated with elevated eye pressure, but pressure is not the whole story. The risk comes from ongoing damage to the nerve fibers that carry visual information to the brain.
One simple way to remember the distinction: cataracts degrade the picture, while glaucoma reduces the signal.
Understanding cataracts
Cataracts usually develop slowly, which is why people often adjust their routines before they realize what is happening. Things like a person using brighter bulbs at home, avoiding night driving, or holding a phone farther away can all signal cataract development.
Cataract symptoms
Cataracts often show up as:
- Hazy or cloudy vision that does not fully clear with blinking
- Glare sensitivity, especially in bright sun or around headlights
- Halos around lights at night
- Reduced contrast, with colors looking less crisp
- Night driving is becoming uncomfortable or tiring
Symptoms tend to progress gradually. Cataracts are also typically painless.
Cataract treatment
Glasses and lighting changes can help early on. A cataract cannot be “medicated away,” though. When it starts interfering with daily activities, cataract surgery removes the cloudy lens and replaces it with a clear intraocular lens (IOL). The goal is functional, comfortable vision, not simply a better eye chart score.
Understanding glaucoma
Glaucoma is often described as “silent,” reflecting how the disease typically progresses. Early stages are often symptom-free–especially in open-angle glaucoma, the most common type.
Glaucoma symptoms
Open-angle glaucoma usually does not cause pain. Early changes can involve subtle, easy-to-miss peripheral vision loss. Many people only recognize it once it has become more advanced.
Angle-closure glaucoma is different and can present suddenly with severe symptoms. Sudden eye pain, nausea, redness, and abrupt blurred vision require urgent evaluation.
Glaucoma treatment
Glaucoma treatment focuses on protecting the optic nerve and reducing the risk of progression by lowering eye pressure. This can be accomplished with prescription drops, laser treatment, or surgery. The goal is stability. Once optic nerve tissue is damaged, vision loss cannot be restored.
Glaucoma vs cataracts vision: how the changes tend to feel
People understandably try to interpret symptoms, but cataracts vs glaucoma is not a DIY diagnosis. Still, patterns can help you understand why a full exam matters.
Cataracts tend to affect image quality. Many people describe it as fog, glare, or a film that can never be fully wiped away. Low-light situations, like night driving, often become the most frustrating first.
Glaucoma tends to affect function at the edges before the center. Early on, central vision can feel “fine,” which is why a simple screening can miss it. Glaucoma is not primarily an eye chart problem at the start. It’s an optic nerve and field-of-vision problem.
How these conditions are diagnosed
While many think of it just as a time to update prescriptions, a comprehensive eye exam evaluates the lens for cataracts and checks structures that matter for glaucoma risk and progression.
Depending on your findings and risk factors, your visit may include an exam of the lens and cornea, measurement of eye pressure, evaluation of the optic nerve, and glaucoma testing, such as visual field testing or optic nerve imaging, when needed.
When to get checked
If you wait for glaucoma symptoms to become obvious, you are often waiting too long. Cataracts usually become noticeable eventually. Glaucoma can progress quietly.
Practical guidance: if you are over 40, have diabetes, have a family history of glaucoma, take steroid medications long term, or have had an eye injury, treat routine comprehensive exams as preventive care. If you already have cataract symptoms that affect driving, work, or safety, schedule an exam soon rather than “pushing through.”
When to seek urgent evaluation
Get prompt care if you experience sudden, severe eye pain, a rapid drop in vision, new flashes of light, a sudden shower of floaters, or a shadow that feels like a curtain in your vision.
Conclusion
Cataracts and glaucoma both become more common with age, but they behave differently and require different timing. Cataracts cloud the lens and usually cause glare, haze, and reduced clarity that gradually worsens. Glaucoma damages the optic nerve and can progress without early warning signs, which makes routine comprehensive exams critical.
If you notice glare, night-driving difficulty, or blurry vision that is not improving, or if you have risk factors for glaucoma, schedule an eye exam with Carolina Eyecare Physicians. A clear diagnosis leads to the right next step, whether that is monitoring, updated lenses, cataract planning, or glaucoma testing and treatment to protect long-term vision.
FAQ: Cataracts vs Glaucoma
Can you have cataracts and glaucoma at the same time?
Yes. They are distinct conditions, and it’s not uncommon to see both in the same patient. In such situations, the care plan depends on which condition is affecting vision most immediately and on the risk factors present.
Does cataract surgery fix glaucoma?
No. Cataract surgery treats the cloudy lens. Some patients may see a modest reduction in eye pressure after cataract surgery, but glaucoma will continue to require close monitoring and treatment
If my vision is blurry, is it more likely cataracts than glaucoma?
Blur and glare often point toward cataracts, dry eye, or refractive error. Glaucoma can exist without noticeable blur early on. The only way to know for sure is a comprehensive exam.
What tests catch glaucoma early?
Eye pressure tests are one piece of a larger set of tools. Doctors also evaluate the optic nerve and may use visual field testing and imaging to identify damage or track subtle changes over time.
Is cataract-related vision loss reversible?
In most cases, yes. Cataract surgery replaces the cloudy lens, and vision often improves significantly once healing is complete.